Author: Adina Lorena Patru | Editor: Laure Pauly, Anja Leist
Menopause is a natural life transition for women, yet for many, it might feel confusing and unpredictable. We tend to associate it with hot flushes, night sweats, mood swings, or changes in sleep. But did you know that the brain also goes through important shifts during this time? These changes can lead to symptoms like the well‑known “brain fog,” temporarily affecting memory, focus, and mental clarity.
What Exactly Is Menopause?
Menopause marks the moment when a woman has gone 12 consecutive months without menstruation. It’s the body’s transition out of the reproductive years and it happens gradually. This transition period is called perimenopause. This period typically unfolds in three stages:
- Early menopause transition: periods become irregular.
- Late menopause transition: menstrual cycles may disappear for 60+ days at a time.
- Early postmenopause: the year following the last menstrual cycle.
During these years, women may experience a wide range of physical, cognitive and psychological symptoms.
Most women reach menopause between 49 and 52, though it can occur earlier or later. A small number experience premature menopause, defined as menopause before age 40.
Brain Fog During Perimenopause: What’s Going On?
If you’ve ever forgotten where you put your keys, blanked on a colleague’s name, or lost your thread mid‑sentence during perimenopause, you’re not alone. These symptoms, often described as brain fog, are known scientifically as cognitive difficulties (1,2,3). Cognition includes mental processes such as memory, attention, organization, planning, and problem‑solving.
Research shows that during perimenopause and early postmenopause, women tend to report more difficulties with:
- Verbal memory (remembering words or stories)
Example: Forgetting the name of a movie you watched last week or mixing up details when retelling a story. - Working memory (holding and manipulating information in the moment)
Example: Doing mental math while cooking, like doubling ingredient amounts, and then suddenly losing track of the numbers. - Executive functions (planning, switching tasks, inhibiting inappropriate responses)
Example: Starting to prepare lunch, then answering a message, then forgetting what you were doing.
It’s important to highlight that these cognitive shifts do not mean dementia is developing. Dementia is a neurodegenerative disease that typically appears after age 65. Many women find their cognition improves again in postmenopause, suggesting that brain fog is temporary and linked to hormonal fluctuations, not permanent decline.
What causes these cognitive changes?
During perimenopause, but also during premature menopause, the body experiences a significant drop in estrogen, a hormone best known for regulating the reproductive system (4). But estrogen does much more than that. It also plays an essential role in the brain, especially in areas involved in memory. When estrogen levels decrease sharply during perimenopause, the communication between certain brain regions can become less efficient. This disruption can lead to these previously described symptoms.
Every woman’s experience is unique. Some notice only mild and occasional changes, while others feel more strongly affected. And it’s not just hormones at play: hot flushes, sleep disturbances, mood fluctuations all common during menopause, can also contribute to cognitive difficulties (2). Some may also experience a dysregulation of their glucose metabolism, with possibly adverse health effects, so it can be good to regularly test blood sugar for irregularities (5).
Effect of hormone therapy on cognition
The use of hormone replacement therapy (HRT) is an interesting avenue since studies point towards the decreasing estrogen being responsible for cognitive difficulties in menopause (1). However, for now, the few studies available are on postmenopausal women only.
There is ongoing research on the new generation of hormone replacement therapies for which we don’t have much evidence on cognition either. The window of opportunity hypothesis says that a woman is more susceptible to benefit from HRT during the perimenopause than during postmenopause. Therefore, there is a window of time during a woman’s life when it would be best to start HRT, but no study has tried to test the effect of HRT during perimenopause on cognitive difficulties yet. Also, we still do not know when exactly this window of opportunity during a woman’s life is.
At the moment, recommendations for cognitive difficulties during the menopausal transition are treating other menopausal symptoms or mental disorders that can contribute to cognitive difficulties and to have a healthy lifestyle that supports cognitive health. Only very few studies have looked at the effect of HRT during perimenopause, but results are only sporadic and not always consistent. Further research is therefore needed to make recommendations.
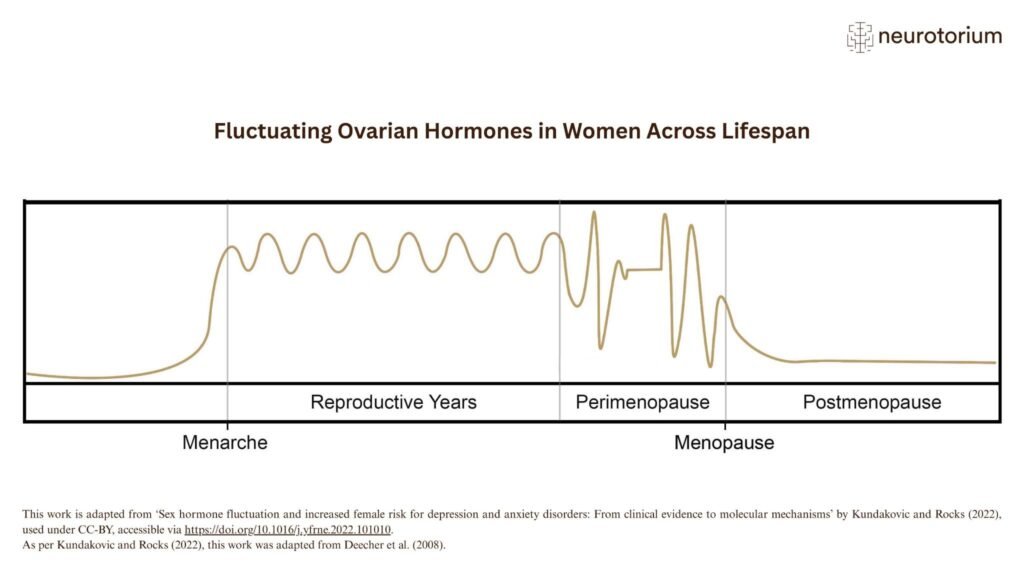
A simplified illustration of ovarian sex steroid fluctuations across the female lifespan, from the first menstrual cycle to menopause. Figure reused with permission under Neurotorium’s creative use guidelines. Copyright notices and the Neurotorium logo remain intact. Source: https://neurotorium.org/article/perimenopause-menopause-and-mental-health/
What can help support brain health during menopause?
At the moment, recommendations for cognitive difficulties during the menopausal transition are treating other menopausal symptoms or mental disorders that can contribute to cognitive difficulties and to have a healthy lifestyle that supports cognitive health. This includes a regular sleep schedule and sufficient hours of sleep (7-9 hours). Physical activity is also an important factor that is associated with quality of life during menopause transition (6). In fact, women that are active during perimenopause reportless cognitive symptoms than those that are inactive (7). Treating other perimenopausal symptoms like hot flashes and sleep disruption through HRT may also help focus and memory by simply reducing the burden of these symptoms.
A stressful life phase even without hormonal changes
Remember that the hormonal changes during perimenopause come during a time when many women are juggling care of children and their aging parents – often mentioned as the “mental load” of organising even if some tasks can be delegated – while often also handling important professional, financial and volunteering responsibilities. A packed schedule and doing many things at the same time can lead to some mistakes. These mistakes – especially if they happen at isolated occasions, after a bad night’s sleep or during extraordinarily busy days – are normal and happen to all of us. However, if you feel worried about their frequency or their intensity, you should seek help or recommendations from a physician or health care provider.
A transition, not a decline
Finally, it is important to remember that experiencing cognitive difficulties during perimenopause is part of the transition that your body is going through. Over half of the people that are going through menopause report cognitive symptoms, meaning that you are not alone. Your body needs some time to adapt to the major decrease of estrogen that is happening. By taking care of your body with a healthy lifestyle, you can minimize menopause symptoms and limit cognitive difficulties. Also, always remember that if you notice a decrease in your cognitive abilities during this period, it is not a sign of early dementia. However, if you are feeling unsure or you have more symptoms that decrease your quality of life, you should always ask for professional help from a qualified physician, especially if you are experiencing premature (before the age of 40) or early (before the age of 45) menopause (8).
If you want to learn more about perimenopause, menopause, and mental health, we recommend the following article: https://neurotorium.org/article/perimenopause-menopause-and-mental-health/
________________________________
Lorena is a guest researcher in Prof. Leist’s group and a PhD student at the University of Montreal in Canada. Her research focuses on the association between age at menopause onset and the risk of late-life cognitive decline. She also investigates the contribution of vascular risk factors, as well as the potential impact of hormone replacement therapy. Passionate about advancing research on women’s health, Lorena is equally committed to making scientific knowledge accessible so that women can be empowered to make informed decisions about their bodies.
________________________________
For better readability of the text, the assistance of Microsoft Copilot, an AI language model based on the GPT-4 architecture, secured with UL enterprise data protection, has been used.
- Maki, P. M., & Jaff, N. G. (2022). Brain fog in menopause: A health-care professional’s guide for decision-making and counseling on cognition. Climacteric, 25(6), 570–578. https://doi.org/10.1080/13697137.2022.2122792
- Metcalf, C. A., Duffy, K. A., Page, C. E., & Novick, A. M. (2023). Cognitive Problems in Perimenopause: A Review of Recent Evidence. Current Psychiatry Reports, 25(10), 501–511. https://doi.org/10.1007/s11920-023-01447-3
- Weber, M. T., Maki, P. M., & McDermott, M. P. (2014). Cognition and mood in perimenopause: A systematic review and meta-analysis. The Journal of Steroid Biochemistry and Molecular Biology, 142, 90–98. https://doi.org/10.1016/j.jsbmb.2013.06.001
- Sochocka, M., Karska, J., Pszczołowska, M., Ochnik, M., Fułek, M., Fułek, K., Kurpas, D., Chojdak-Łukasiewicz, J., Rosner-Tenerowicz, A., Leszek, J., Sochocka, M., Karska, J., Pszczołowska, M., Ochnik, M., Fułek, M., Fułek, K., Kurpas, D., Chojdak-Łukasiewicz, J., Rosner-Tenerowicz, A., & Leszek, J. (2023). Cognitive Decline in Early and Premature Menopause. International Journal of Molecular Sciences, 24(7).
- Geraets, A., Ford, K., May, P., Kidd, E., & Leist, A. (2025). Associations of age at menopause, bilateral oophorectomy, hysterectomy and hormone replacement therapy with glycaemia and risk of dementia: a study based on the population-based UK Biobank cohort. BMJ Public Health, 3(2).
- Mansikkamäki, K., Raitanen, J., Malila, N., Sarkeala, T., Männistö, S., Fredman, J., Heinävaara, S., & Luoto, R. (2015). Physical activity and menopause-related quality of life – A population-based cross-sectional study. Maturitas, 80(1), 69–74. https://doi.org/10.1016/j.maturitas.2014.09.009
- Anderson, D., Seib, C., & Rasmussen, L. (2014). Can physical activity prevent physical and cognitive decline in postmenopausal women?: A systematic review of the literature. Maturitas, 79(1), 14–33. https://doi.org/10.1016/j.maturitas.2014.06.010
- Hamoda, H., & Sharma, A. (2024). Premature ovarian insufficiency, early menopause, and induced menopause. Best Practice & Research Clinical Endocrinology & Metabolism, 38(1), 101823. https://doi.org/10.1016/j.beem.2023.101823



